Contraception Methods Compared: Which One Is Right for You?
- Asele Team
- Apr 23
- 5 min read

Choosing a birth control method can feel overwhelming. There are pills, patches, injections, implants, IUDs, condoms — the list goes on. And each option comes with its own set of pros, cons, and side effects.
This guide breaks down the most common contraceptive methods so you can have an informed conversation with your healthcare provider about what's right for you.
tldr:
There's no single 'best' contraceptive; it depends on your body, your lifestyle, and your plans. IUDs and implants are the most effective (99%+), the pill works well if taken consistently, and condoms are the only method that also protects against STIs.
Quick Comparison Table
Method | Effectiveness (typical use) | How Long It Lasts | Protects Against STIs? |
Hormonal IUD | 99%+ | 3–8 years | No |
Copper IUD | 99%+ | Up to 10 years | No |
Implant | 99%+ | 3–5 years | No |
Injectable (Depo-Provera) | 94% | 3 months | No |
Combined Pill | 91% | Daily | No |
Mini-Pill (progestin only) | 91% | Daily | No |
Patch | 91% | Weekly | No |
Vaginal Ring | 91% | Monthly | No |
Male Condom | 82% | Single use | Yes |
Female Condom | 79% | Single use | Yes |
Effectiveness rates reflect typical use, meaning how well the method works in real life (including occasional mistakes like missing a pill).
Long-Acting Methods (Set It and Forget It)
The Hormonal IUD

A hormonal IUD is a small, T-shaped plastic device placed inside your uterus by a healthcare provider. It releases a small amount of progestin (a synthetic version of the hormone progesterone) directly into your uterus.
Pros:
Extremely effective (over 99%)
Lasts 3 to 8 years depending on the brand
Often makes periods lighter and less painful
You don't have to remember to take anything daily
Cons:
Insertion can be uncomfortable or painful
Some women experience irregular bleeding or spotting in the first few months
Requires a healthcare provider for insertion and removal
Does not protect against STIs (sexually transmitted infections)
The Copper IUD

Similar to the hormonal IUD in shape, but uses copper instead of hormones. The copper creates an environment that's toxic to sperm.
Pros:
Hormone-free — good for women who can't or don't want to use hormones
Lasts up to 10 years
Can be used as emergency contraception if inserted within 5 days of unprotected sex
Cons:
May cause heavier, longer, or more painful periods
Insertion can be painful
In Sub-Saharan Africa, copper IUD use is very low (under 2% of contraceptive users in most countries), partly due to limited availability and provider training
The Contraceptive Implant

A small, flexible plastic rod (about the size of a matchstick) inserted under the skin of your upper arm. It releases progestin.
Pros:
Over 99% effective
Lasts 3 to 5 years
You can't feel it working — nothing to remember daily
Quickly reversible once removed
Cons:
The most common side effect is irregular bleeding, especially in the first 6 to 12 months
Some women stop having periods altogether (which is safe but can be unsettling)
May cause headaches or breast tenderness
In some African countries like South Africa, negative experiences with irregular bleeding led to widespread discontinuation of implants
Short-Acting Hormonal Methods
The Combined Pill

Contains both estrogen and progestin. You take one pill at the same time every day.
Pros:
Can regulate periods, reduce cramps, and improve acne
You have control — you can stop anytime
Also reduces the risk of ovarian and endometrial cancer
Cons:
Must be taken at the same time every day — missing pills reduces effectiveness
Side effects can include nausea, breast tenderness, headaches, and mood changes
Slightly increases the risk of blood clots, especially in women who smoke or are over 35
Not recommended for women with certain conditions like high blood pressure or a history of blood clots
The Progestin-Only Pill (Mini-Pill)

Contains only progestin, no estrogen.
Pros:
Can be used by women who can't take estrogen (including breastfeeding mothers)
Fewer cardiovascular risks than the combined pill
Cons:
Must be taken at the same time every day — even a 3-hour delay can reduce effectiveness
More likely to cause irregular bleeding than the combined pill
The Injectable (Depo-Provera)

A progestin injection given every 3 months by a healthcare provider.
Pros:
Only needed every 12 weeks
Very popular in many African countries due to accessibility
Can reduce period pain and heavy bleeding
Cons:
May cause weight gain (a common concern among users)
Can take 6 to 12 months for fertility to return after stopping
May reduce bone density (the strength of your bones) with long-term use
Cannot be reversed once injected — you must wait for it to wear off
The Patch and the Vaginal Ring
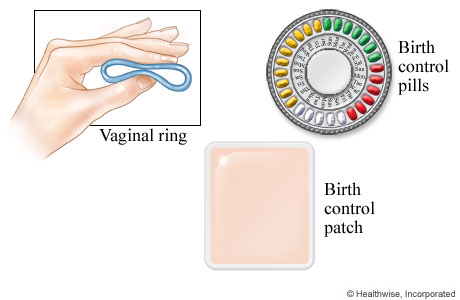
The patch is worn on the skin and changed weekly. The vaginal ring is inserted into the vagina and replaced monthly. Both release estrogen and progestin.
Pros:
Less daily effort than the pill
Similar effectiveness and benefits to the combined pill
Cons:
The patch may irritate the skin
The ring may cause vaginal discomfort
Limited availability in many African countries
Barrier Methods
Male Condoms

Pros:
The only method (besides female condoms) that protects against both pregnancy and STIs, including HIV
Widely available, affordable, and don't require a prescription
No hormonal side effects
Cons:
Must be used correctly every time
Can break or slip
Some people are allergic to latex (non-latex options are available)
Female Condoms

Pros:
Woman-controlled — you don't need your partner's cooperation
Protects against STIs
Can be inserted up to 8 hours before sex
Cons:
Less widely available
Takes practice to use correctly
Slightly less effective than male condoms
Emergency Contraception
Emergency contraception (also called the "morning-after pill") is not a regular contraceptive method, but it's important to know about.
Options include:
Levonorgestrel pill (Plan B) — Most effective within 72 hours of unprotected sex
Ulipristal acetate (ella) — Effective up to 5 days after
Copper IUD — The most effective form of emergency contraception if inserted within 5 days
Emergency contraception is not an abortion pill. It prevents pregnancy from occurring — it does not end an existing pregnancy.
How to Choose
Consider these questions:
Do you want something long-term or short-term? If you don't want to think about contraception daily, an IUD or implant may be ideal.
Do you need STI protection? If yes, condoms should be part of your plan, even if you use another method.
Do you want to avoid hormones? The copper IUD and condoms are your hormone-free options.
Are you planning to get pregnant soon? Methods like the pill, patch, ring, condom, and implant allow for a quick return to fertility. The injectable may take longer.
Do you have any health conditions? Certain methods aren't recommended for women with specific conditions. Always discuss your medical history with your provider.
Contraception Access in Africa
Access to contraception varies widely across the continent.
Injectables are the most commonly used method in many Sub-Saharan African countries, partly due to availability and the fact that they can be administered by community health workers. Implant use has been growing rapidly in countries like Kenya, Senegal, and Ghana.
However, barriers remain — including cost, provider shortages, cultural stigma, and misinformation. If you're struggling to access contraception, local family planning clinics can help.
The Bottom Line
There is no single "best" contraceptive. The best method is the one that fits your body, your life, and your goals. Talk to a healthcare provider, ask questions, and don't settle for a method that makes you feel bad. You have options.
References
CDC. "Contraception and Birth Control Methods." cdc.gov
ACOG. "Effectiveness of Birth Control Methods." acog.org
JAMA. "Contraception Selection, Effectiveness, and Adverse Effects: A Review." jamanetwork.com
Cleveland Clinic. "Birth Control Options." clevelandclinic.org
Marie Stopes South Africa. "IUD Birth Control." mariestopes.org.za



Comments